
You have made it through winter. The worst of it, the cold air, the central heating, the layers that scratch. And then spring arrives and somehow your child’s skin gets worse, not better.
If that sounds familiar, you are not imagining it. For many children with eczema, spring is actually the hardest time of year. And hay fever is often why.
Are eczema and hay fever connected?
They are, more closely than most parents realise.
Children with eczema are more than twice as likely to develop hay fever compared to children without it. This is not bad luck. Both conditions share the same underlying immune pattern, what doctors call the atopic march: eczema tends to arrive first, often in infancy, and hay fever follows as the immune system finds new things to react to.
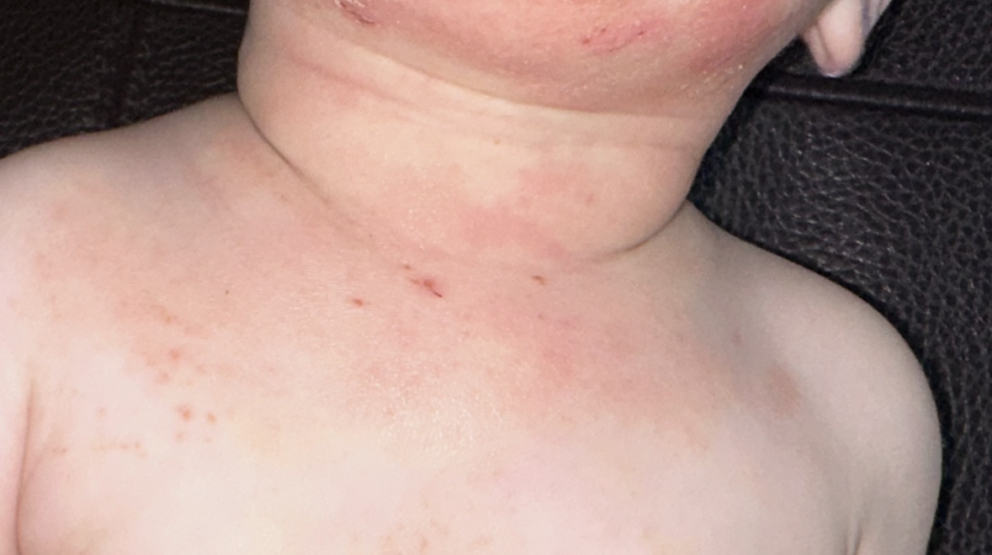
When both conditions are present in the same child, they amplify each other. Pollen does not just cause a streaming nose and itchy eyes. In children with sensitised skin, it sets off an inflammatory response that shows up on the skin too.
Why does pollen make eczema flare?
Eczema in children weakens their skin barrier more than children without it. That means airborne allergens like pollen can get through more easily, activating an immune response that, in an already sensitised system, is fast and intense.
Two things are happening at once. Pollen inhaled through the nose and airways triggers a body-wide inflammatory response, releasing histamine and starting the itch-scratch cycle. At the same time, pollen landing directly on exposed skin triggers a localised reaction on the surface. Both channels are active simultaneously.

1 in 3
Pollen counts peak in the early morning and late afternoon. Mid-morning and after rainfall are safer windows for outdoor time.
A lukewarm shower removes pollen from hair and skin. It does not need to be a long bath. The habit matters more than the duration, especially through May and June when grass pollen is at its highest.
Overnight pollen exposure matters because histamine response peaks at night. That is partly why scratching is hardest to manage between midnight and 4am. Keeping the bedroom window closed from late afternoon helps reduce what your child is breathing in while they sleep.
Exposed skin during high-pollen conditions is skin that can react. Lightweight long-sleeved layers act as a physical barrier between your child’s skin and airborne allergens, reducing both direct pollen contact and the heat and friction that make allergic flares worse.
The fabric matters here. Rough textures, synthetic fibres, and tight fits all add mechanical irritation on top of an already active immune response. HappySkin garments are made from Tencel Cotton and treated with DreamSkin Technology, a patented polymer coating with clinically proven anti-inflammatory properties. Unlike barrier creams, DreamSkin manages moisture without blocking pores, allowing skin to breathe while it works. For children prone to pollen-season flares, wearing HappySkin through peak months reduces both allergen contact and the conditions that make flares escalate.

Which HappySkin products help most during pollen season?
Most parents focus on what their child eats, where they play, and what creams to use. Clothing for sensitive skin is often the last thing considered, but it is the one thing in contact with their skin every hour of the day.
During peak pollen months, the right garment acts as a physical barrier between sensitised skin and the air around it, while the wrong one adds friction, heat, and irritation on top of an already active immune response. DreamSkin Technology works the way a healthy skin barrier should: managing moisture, supporting the skin’s own repair response, and letting it breathe rather than sealing it off.
If your child’s skin tends to flare between March and July, our spring and summer range is a good place to start.
All HappySkin garments are dermatologist recommended and designed to be worn directly against the skin.
A word on the atopic march
If your child had eczema as a baby and is now developing hay fever, it can feel like things are heading in the wrong direction. Understanding the atopic march takes some of the alarm out of that, even if it does not make the day-to-day easier.
The atopic march describes the typical progression from eczema in infancy toward hay fever and sometimes asthma in later childhood. Not every child follows this path. But knowing it exists means you can watch for early signs and respond to them, rather than waiting until symptoms are already severe.
Addressing hay fever early, through allergen reduction, through medical support, through clothing that limits how much pollen reaches the skin, reduces the inflammatory load that makes eczema harder to control. Both conditions share the same immune pathway. Managing them together gives your child a better chance at comfortable skin through the months when pollen is at its highest.
REFERENCES
- Allergy UK. Statistics and Figures. allergyuk.org
- Bosma AL et al. Journal of Dermatology. 2021. doi:10.1111/1346-8138.15750
- Gov.uk. Hay fever and airborne allergens. 2025.
- Met Office UK Pollen Forecast. metoffice.gov.uk
Our products
Related Posts











