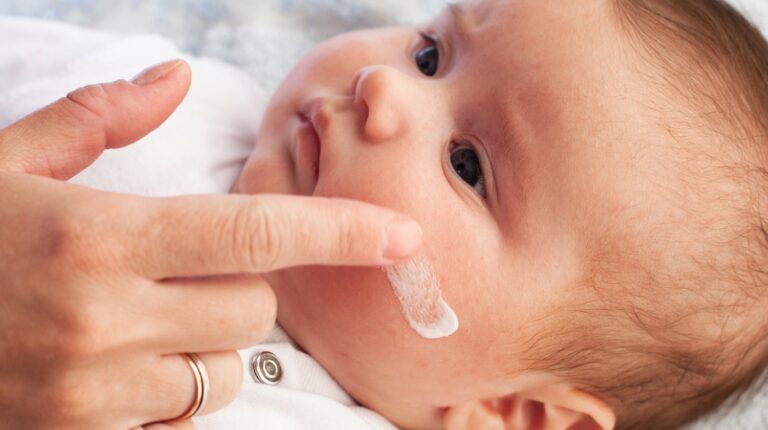
Night-time is one of the most persistent challenges in childhood eczema.

Why does eczema often feel worse at night?
While symptoms could appear manageable during the day, many parents notice a clear pattern of worsening discomfort after bedtime. This is not random. It reflects the interaction between skin barrier weakness, immune rhythm, temperature shifts and unconscious scratching during sleep. Understanding what changes at night is the first step towards reducing both itch intensity and skin damage.
Eczema can feel more intense at night due to a combination of biological and environmental factors.
Inflammatory activity follows a daily rhythm. Certain hormones that help regulate inflammation, such as cortisol, naturally fluctuate overnight. Lower anti-inflammatory activity during sleep may increase itch sensitivity in already reactive skin.
Body temperature increases slightly during sleep. Under bedding, local heat and mild sweating can further disrupt the fragile eczema barrier.
When skin becomes warmer, water loss through the barrier can increase. In eczema-prone skin, where the barrier is already compromised, this additional moisture loss can intensify dryness and itch signaling.

Night-time worsening does not necessarily mean the eczema is globally deteriorating. It often reflects predictable physiological shifts.
Why do children scratch more during sleep?
Scratching at night is frequently subconscious. Even if a child falls asleep comfortably, itch signals can trigger automatic motor responses.
During lighter sleep phases, small repetitive movements may occur without full waking. In eczema-affected skin, even mild friction can:
- Disrupt the outer barrier further
- Increase local inflammation
- Prolong the itch–scratch cycle
Because this scratching happens without awareness, simply telling a child to “stop scratching” is rarely effective. Protection and inflammation control are more realistic strategies than behaviour suppression alone.

What makes night-time scratching more damaging?
Several factors amplify skin trauma overnight:
Wrists, ankles and neck areas may rub repeatedly against bedding.
During eczema flare-ups, the skin struggles to regulate temperature efficiently. Occlusive creams such as paraffin-based ointments can trap sweat and prevent evaporation. The ammonia, urea and salts in sweat may then aggravate already inflamed skin, leading to further irritation and potential sleep disruption.
Inflamed skin is structurally weaker and more vulnerable to micro-tears.

This combination explains why some children wake with visibly worsened patches despite appearing settled at bedtime.
How should night-time eczema be managed?
Management should follow a structured hierarchy rather than isolated quick fixes.
- Control active inflammation first
Persistent night itching is often a sign of undertreated inflammation. If a flare is present, prescribed anti-inflammatory treatment should be used appropriately alongside moisturising. Barrier protection alone will not calm inflamed skin.
- Optimise evening barrier repair
Apply emollients generously before sleep. Well-hydrated skin is less prone to cracking and irritation overnight.
- Regulate temperature
Keep bedrooms cool and well ventilated. Avoid excessive layering. Overheating is one of the most common aggravators of night itch.
- Reduce friction and mechanical trauma
Where unconscious scratching is frequent, protective strategies may help reduce skin damage.
These can include:
- Soft, breathable eczema gloves
- Scratch-reducing sleeves
- Carefully designed eczema-friendly sleepwear
The goal is not restriction, but reducing sharp nail trauma and repetitive friction.
Do eczema gloves help at night?
Eczema gloves do not treat inflammation directly. Their role is protective.
Potential benefits include:
- Minimising skin breakage from sharp nails
- Reducing secondary infection risk
- Limiting friction against inflamed areas
For overnight use, breathability is critical. Gloves that trap heat or moisture may worsen itching. The most effective designs prioritise airflow and comfort while limiting mechanical damage.
Protective gloves are best viewed as a supportive layer within a broader eczema management plan, not a standalone solution.
What type of sleepwear is suitable for eczema-prone children?
Night-time fabrics influence both temperature regulation and friction.
Key characteristics to look for include:
- Lightweight, breathable materials
- Smooth surfaces to minimise rubbing
- Flat seams to reduce irritation points
- A secure but non-restrictive fit
Clothing that traps heat or causes localised rubbing around wrists, ankles or the neck may aggravate itching. In contrast, well-designed sleepwear for eczema can help maintain a more stable overnight environment for vulnerable skin.
Sleepwear should support, not replace, appropriate medical and moisturising treatment.
Read More: Eczema Guide for Babies and Children: Symptoms, Causes and Treatment

What should a structured night routine include?
A consistent routine improves predictability and reduces reactive decision-making.
A balanced approach may include:
- Gentle evening cleanse if part of usual care
- Pat skin dry without rubbing
- Apply moisturiser generously
- Dress in breathable, low-friction sleepwear
- Maintain a cool bedroom environment
If night waking due to itch is frequent despite these steps, medical review may be necessary.
When should persistent night itching be medically reviewed?
Medical advice should be sought if:
- Night scratching repeatedly breaks the skin
- Signs of infection develop
- Sleep disruption is severe or ongoing
- Prescribed treatments are not improving control
Persistent night itching often indicates that inflammation requires reassessment rather than additional moisturiser alone.
Frequently Asked Question
Not always, but many children experience increased itch sensitivity overnight due to temperature and circadian factors.
Soft, breathable gloves designed for eczema can be used overnight if they do not cause overheating.
Better sleep may support overall wellbeing, but controlling inflammation and protecting the skin barrier remain primary priorities.
Sleepwear influences both temperature regulation and friction.
Suitable pyjamas for eczema-prone skin typically:
- Minimise seam irritation
- Reduce repetitive rubbing
- Avoid excessive heat retention
- Allow airflow
Poorly designed fabrics may trap warmth or increase friction, aggravating symptoms. Carefully designed eczema-friendly sleepwear can support a more stable overnight environment.
Sleepwear is supportive, not curative.
Sedating antihistamines are sometimes prescribed to improve sleep in children with severe itching. However, they do not directly treat the underlying inflammation.
Medical guidance is required before using any oral medication for night-time itch.
Not always. Even mild eczema can feel disproportionately worse at night due to physiological factors.
However, persistent night waking, repeated skin breakage or poor response to treatment may indicate more active inflammation and warrant review.
Clinical References and Further Reading
Guidance on atopic dermatitis management is available from:
- National Institute for Health and Care Excellence (NICE)
- NHS guidance on eczema in children
- American Academy of Dermatology (AAD)
These sources emphasise barrier repair, appropriate anti-inflammatory treatment and trigger management as the foundation of eczema control.