
For many living with eczema, topical steroids, hydrocortisone and paraffin creams have long been considered a frontline treatment. But what happens when your skin stops responding and starts reacting?
A growing number of individuals report distressing symptoms after stopping steroids – symptoms that often feel worse than their original skin condition. This reaction is known as Topical Steroid Withdrawal (TSW), sometimes called ‘red skin syndrome’ or ‘topical steroid addiction’.
You followed every instruction. You applied the cream when the GP said so. And now your child’s skin looks worse than it ever did before treatment, the redness deeper, the itching constant, the burning new. If you suspect this is more than another flare, you may be looking at topical steroid withdrawal.
TSW is real, it is increasingly recognised by clinicians and regulators in the UK, and it is exhausting for any family living through it. In our work with thousands of eczema families, we have noticed that TSW often goes misdiagnosed as a worsening eczema flare for weeks before the pattern becomes clear. The cream that used to help stops working. The flare spreads further than usual. The skin starts to burn rather than itch. By the time families piece these signs together, they have often been through months of confusion.
This guide walks you through what TSW actually is, how to tell it apart from an eczema flare, and the practical steps families have used to support their child through recovery. We have written it as the kind of article we wish had existed when parents first started reaching out to us about it.
What Is Topical Steroid Withdrawal?
Topical Steroid Withdrawal, sometimes called red skin syndrome or topical steroid addiction, is a reaction some people experience after stopping the long-term use of corticosteroid creams. The symptoms can appear shortly after the cream is stopped, and they often affect skin areas where steroids were never even applied. This is one of the clues that distinguishes TSW from a typical eczema flare.
TSW is most commonly associated with prolonged use of moderate or high-potency steroids, but in children it has been reported even after relatively short courses. While the medical research around it is still developing, patient advocacy and clinical reports have brought it firmly into mainstream conversation. The Medicines and Healthcare products Regulatory Agency issued an official safety warning about it in 2021, and the British Association of Dermatologists has published a joint statement acknowledging it as a real phenomenon.

Signs and Symptoms of Topical Steroid Withdrawal
What does topical steroid withdrawal look like? TSW symptoms often differ from a traditional eczema flare-ups. Some of the most reported include:
- Persistent redness or flushing (“red skin syndrome”)
- Deep burning or stinging sensations
- Intense itching or crawling skin
- Weeping, flaking, or shedding
- Swelling, especially around eyes and joints
- Insomnia or anxiety triggered by skin discomfort
- A sensation of tight, paper-thin skin
- Oozing lesions or patches that appear suddenly
These symptoms often cycle, meaning they can appear in waves or flare-ups, lasting days to weeks. People frequently note that areas previously unaffected by eczema can become inflamed during withdrawal.
How to Tell TSW Apart from an Eczema Flare
The two can look strikingly similar at first. Redness, itching, dryness, broken skin. But the underlying patterns are different, and recognising them early matters because the response is also different. Continuing to treat TSW as if it were a regular flare can prolong it. Below is the comparison families have told us was the most useful thing they read.
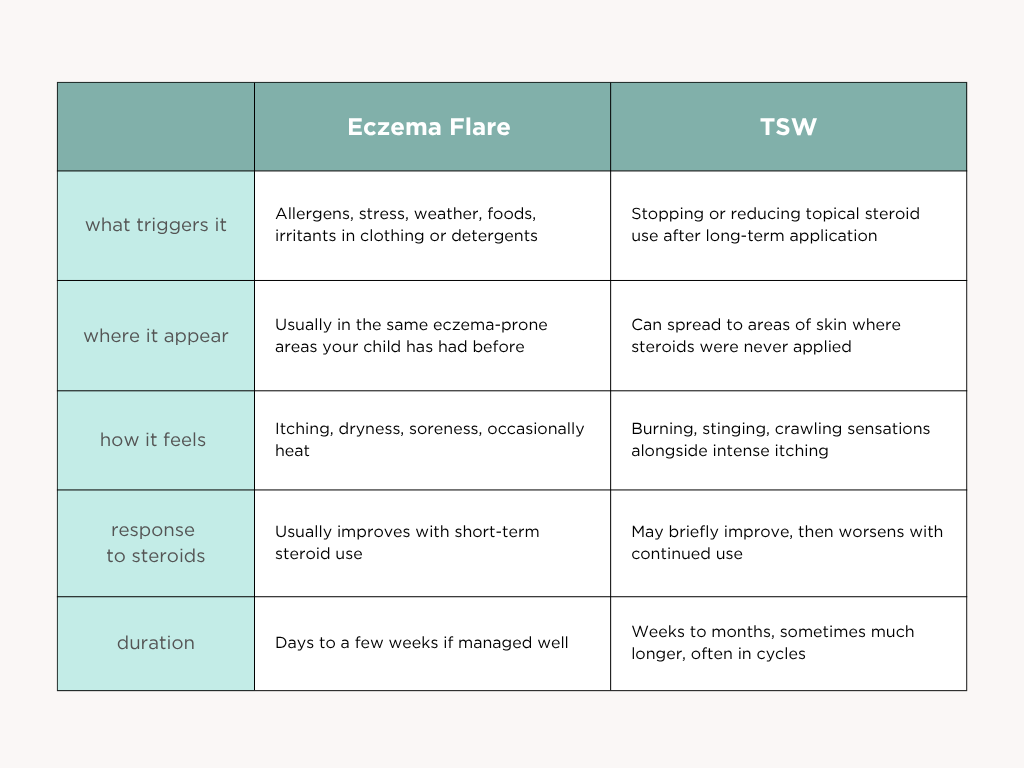
Parents who reach out to HappySkin often describe the same moment of realisation. The skin reacts to the cream that used to help. The flare spreads further than usual. The burning sensation is something new, something they have not seen before in years of managing eczema. If this is what you are seeing, take it seriously. The earlier TSW is recognised, the more support you can put in place.
How TSW Looks in Children Specifically
Most online resources about TSW are written for adults, but children’s skin reacts differently. TSW in young skin can present with widespread redness, weeping patches, and a sensitivity that makes ordinary clothing or even bath water painful. Sleep is almost always affected. Many parents tell us their child wakes every two hours scratching, exhausted but unable to settle, with the burning sensation that defines TSW being worse at night when the body is warm and still.
Behavioural changes can be one of the first clues. A child who suddenly resists bath time, who refuses certain clothing they used to be fine with, or who cannot bear being held the way they used to, may be telling you their skin hurts in a way they cannot explain. Younger children especially struggle to articulate the difference between the familiar itch of eczema and the new burning of TSW.
Research has shown that TSW in children can occur after as little as two months of steroid use, with symptoms lasting more than 12 months even when the original steroid use was relatively short. This duration is one of the hardest parts for families to accept. Recovery is real, but it is not quick, and it rarely follows a straight line.
When Autumn Brings Itching Skin Allergies: Managing Eczema Flares Without Creams or Steroids

What to Do If You Suspect Your Child Has TSW
The steps below are what families have found most useful. They are not medical advice, and they are not a substitute for your GP, but they are a practical starting point that you can begin today while you wait for an appointment.
Take photos of your child’s skin every day, or at least every few days, in the same lighting conditions. Natural daylight near a window works best because it shows colour accurately. Note when steroids were used, when they stopped, and how the skin changed in response. This timeline becomes the most useful single thing you can bring to a GP appointment, particularly if your GP is not yet familiar with TSW. A photo log makes the pattern undeniable in a way that verbal descriptions cannot.
Stopping steroids suddenly can make things worse. If you suspect TSW, do not pull the cream cold. Bring your photos and timeline to your GP and ask about a tapering plan. If your GP is unfamiliar with TSW, request a referral to a dermatologist who has experience with it. ITSAN and Eczema Outreach Support both maintain helpful resources you can print and share with your healthcare team. Coming to the appointment prepared, with documented evidence and informed questions, often changes how the conversation goes.
Many traditional emollients prescribed for eczema are paraffin-based. During TSW, these can prolong recovery by trapping heat against already inflamed skin and creating a sealed barrier that the skin cannot breathe through. A non-paraffin recovery cream allows the skin to manage moisture without being suffocated. Avoid fragranced products, harsh cleansers, exfoliants, and anything labelled as anti-bacterial or medicated unless specifically recommended by a dermatologist familiar with your child’s case.
Clothing becomes part of the treatment plan during TSW because it is the one thing that stays in contact with the skin for 24 hours a day. We cover this in detail in the next section, but the short version is that friction makes TSW worse.
Night-time scratching can undo a week of healing in a few hours. Cool the bedroom slightly, choose breathable bedding without synthetic fibres, and use full-coverage clothing or scratch-protection garments where the skin is most affected. Our guide on eczema itching at night goes into the science of why night-time itching feels worse and how families have managed it during the worst stretches of recovery.
TSW is isolating in a way that few other skin conditions are, partly because it is still misunderstood and partly because the recovery is so long. Connecting with other parents going through the same thing changes how it feels to face a 12-month journey. ITSAN, Eczema Outreach Support, and the National Eczema Society all have active communities. Our HappyClub also brings parents together to share what is working day to day, and many of our most useful insights as a brand have come from those conversations.
Steroid-Free Cream for Irritated Skin
Why Clothing Matters During TSW Recovery
Most TSW articles focus on creams, diet, and supplements. Clothing is often treated as an afterthought, mentioned briefly with generic advice to choose soft fabric. From our years of working with eczema families, we believe this misses something important. Clothing is the only treatment that touches the skin for 24 hours a day. During TSW, when steroids and many creams are off the table or being used only sparingly, clothing can become one of the most important tools you have.
Clothing as 24-hour scratch protection
Scratching during TSW is often unconscious and happens most during sleep, which is why families lose so much sleep alongside their child. Full-coverage garments, such as long-sleeve bodysuits, leggings, sleepsuits and pyjamas, reduce direct contact between fingernails and inflamed skin. This breaks the scratch-damage cycle that prolongs every flare and gives the skin its best chance to heal between waves.
Pieces that families have found most useful for TSW
Different children need different combinations depending on where the TSW is most active. Eczema sleepsuits and pyjamas give full overnight coverage when scratching is at its worst, which is the single most disruptive part of the condition for most families. A head mask helps with facial TSW, which is one of the most distressing presentations because it is visible and because the skin on the face is so thin. Eczema gloves are useful when the hands are involved or when scratching damage is concentrated there. For families wanting a complete solution, our Severe Eczema Treatment Packs cover both day and night with the right pieces matched to severity level.
How Long Does TSW Last?
This is the question parents fear asking, because the honest answer is rarely the one they hope for. For some children, symptoms ease within a few months. For others, full recovery takes 12 to 24 months, sometimes longer, often in cycles of improvement and setback that can feel demoralising when you are in the middle of them.
Recovery depends on several factors: the strength and duration of steroid use, the body areas affected, your child’s age, and how well the skin is supported during withdrawal. The skin almost always returns to normal in time, but the path is not linear. Knowing this from the start helps you set realistic expectations, recognise that a setback is part of the pattern rather than a failure, and avoid losing hope when progress feels slow.
Some children come out of TSW with skin that is more sensitive than before, particularly to sunlight, heat, or certain fabrics. This sensitivity often softens over time but can persist for months after the visible symptoms have settled. Building a long-term, gentle routine matters even after the worst is over.
When to See a Doctor Urgently
TSW itself is generally not a medical emergency, but inflamed skin can be vulnerable to other problems that are. Contact your GP urgently or call 111 if you notice any of the following:
- Yellow or green crusting, pus, or discharge that smells unusual, which can indicate a secondary infection that needs antibiotics
- A fever that develops alongside skin symptoms, particularly if your child seems unwell beyond what the skin alone would explain
- Swelling around the eyes that affects vision, makes the eyes hard to open, or causes obvious distress
- Your child becoming withdrawn, refusing food or fluids, or showing signs of severe distress that you cannot soothe
- Cracked or bleeding skin that is not healing, is spreading rapidly, or is producing fluid that has changed in appearance
Trust your instinct here. Parents almost always know when something has shifted from difficult to dangerous, and no GP will mind being called for what turns out to be a false alarm.
TSW is not yet listed in every dermatology guideline, but it is increasingly recognised by clinicians, patients, and regulators. The Medicines and Healthcare products Regulatory Agency issued a safety warning in 2021, and the British Association of Dermatologists has published a joint statement acknowledging it as a real phenomenon. Awareness is growing year on year, and most UK dermatologists today have at least encountered it, even if their familiarity varies.
Yes. While TSW is more commonly reported in adults, research has shown it can occur in children after as little as two months of moderate to high-potency steroid use. Symptoms can last more than 12 months, sometimes longer, even when the original steroid course was relatively short. Children may also struggle more than adults to describe what they are feeling, which can delay diagnosis.
If your child’s skin became dramatically worse after stopping or reducing steroids, particularly with new burning sensations or spreading to areas that never had eczema before, TSW is worth discussing with your GP. The comparison table earlier in this article covers the main differences. Photographic documentation over time also helps make the pattern clearer.
Most children recover their normal skin function with time. The skin barrier can take many months to rebuild, and there may be lasting sensitivity to triggers like sunlight, heat, or fragrance. Recovery is real, but it is rarely linear, and the timeline can be longer than parents expect. Setbacks during recovery do not mean recovery is not happening.
Clothing cannot cure TSW, but it can reduce friction, prevent scratching damage during sleep, and avoid the additional irritation that comes from standard fabrics, detergent residues, or barrier creams that trap heat. For families during a 12-month recovery, this matters every day. Clothing is one of the few things you can control completely while waiting for the skin itself to heal.
Most cases resolve without permanent scarring. Prolonged inflammation and scratching can cause hyperpigmentation, temporary scarring, or skin thickening, but these usually fade over the months and years that follow. Protecting the skin during the active recovery phase, particularly from scratching damage, reduces the risk of any lasting marks significantly.
TSW Recovery with Therapeutic Clothing
Sign up to Happy Club
To get the latest news, promotions, and discounts first, please join our mailing list.
Simply enter your email below!













